

This is a story about missed diagnosis after missed diagnosis, a persistent patient, and finally some answers that brought substantially improved health. It brings home a certain unsteadiness about diagnosing disorders like chronic fatigue syndrome and POTS (Postural Orthostatic Tachycardia Syndrome) that’s both unsettling and exciting. It’s also a cautionary tale for anyone predisposed to rely solely upon what doctors say.
This story goes in our ‘alternate diagnoses’ basket where what appears to be ME/CFS/FM (or in this case POTS) also turns out to be something else, and thankfully so.
Alternate Diagnoses
The story of Lauren Stiles’s (or POTSgrrl on her blog) physical breakdown is all too familiar. An athletic, outgoing, and energetic environmental attorney, Lauren woke up sick on Jan 2, 2010 (yes, she remembers the exact date) in the middle of a ski trip. Besides skiing, she enjoyed surfing, kayaking, and mountain biking. She was the furthest thing from a couch potato you could imagine, but on Jan 2, 2010 her body quickly and dramatically fell apart. She went from snowboarding to barely able to stand in four days.
Upon standing, Lauren’s heart rate would rise from 60-80 bpm to about 130 bpm. At its peak it could hit a dangerously high 230 bpm. While she was in the hospital for two months, the doctors were so alarmed at her escalating heart rate that they kept her bedridden. (The forced bed rest made her symptoms worse, by the way.)
From time to time she would faint; luckily she often had warning signs (see below) before fainting that would allow her to sit down first.
“I get lightheaded, dizzy, off-balance feeling, my vision gets grayed out or blurry or tunnel vision, I feel like my blood is being flushed downwards to my feet, my legs feel heavy, like I’m wearing cement shoes, and I usually get a bit sweaty on my upper body, I feel shaky and I feel short of breath.”
Her symptoms didn’t cease when she would lie down. Her pounding heart was so loud when she would lie down to sleep that she had to turn the TV up loud to distract her from the sound of her heart. At times her throbbing pulse appeared to be flashing in her eyes, and she suffered from vertigo even when lying down. Acid reflux didn’t help matters.
Nerve damage left her with tingling, numbness, cold feelings, too little or too much sweating, pain, blotchy purple skin color, swelling in her lower arms and legs upon standing, and more.

Healthy and athletic, Lauren, four days after being struck down by her mystery disorder, Lauren was unable to walk
If that wasn’t enough there was the diarrhea and vomiting several times per day, which lead to an extreme weight loss (more than 50 pounds in three months), plus hypersensitivity to pain and touch, noise, and odors. She was easily startled, experienced flushing and hives almost everyday, and had a new onset of food allergies and lactose intolerance. She had a “pins and needles” feeling, unevenly dilated pupils, spaciness, difficulty focusing, and “brain fog.”
Like many people with POTS, she was so lightheaded, at times she could barely walk from her bed to the bathroom.
This lady was in bad shape! Like most people with her collection of symptoms, she was misdiagnosed frequently before she got to the heart of the matter. Lauren was misdiagnosed with Irritable Bowel Syndrome, Chronic Fatigue Syndrome, Fibromyalgia, Myofascial Pain Syndrome, Addison’s, Carcinoid Syndrome (which is a form of neuroendocrine cancer), and “it’s just stress, have a glass of wine.” After getting the runaround for nine months, Lauren was finally diagnosed with autonomic neuropathy and POTS. It turned out that her POTS/autonomic neuropathy diagnosis was preliminary–just the beginning of a longer search that ended up with yet another diagnosis.
The Search
“The internet may have saved my life.” -POTSgrrl
Like many young women with POTS, Lauren was initially misdiagnosed as having an anxiety disorder, and indeed she noted that some of the symptoms associated with POTS can look like a ‘permanent anxiety attack.’These symptoms, such as tachycardia when standing, shortness of breath, and an increased sensitivity to pain are caused by a combination of low blood volume, blood pooling in the lower body, excessive plasma norepinephrine, and a denervation hypersensitivity caused by damaged small nerve fibers. When researchers separate out the physical symptoms associated with POTS, and look for the cognitive symptoms of anxiety, POTS patients actually have lower rates of anxiety and panic disorder than healthy controls.
Most of her doctors took her seriously, but she also met up with some “amateur psychologists” among the doctors. One MD decided her fainting, chest pains, , swollen lymph glands, night-sweats and drastic weight loss were simply her way of telling her husband that she wanted kids. This MD ignored the fact that she was a busy career woman who was active in politics, served on several non-profit boards, and who put herself and her husband through graduate school.
- Check out ‘Maggie’s Panic’ – Dr. Bells story of a young woman diagnosed with anxiety disorder who actually had low blood volume.
Despite being located just outside of New York City and seeing some of the best doctors at the best hospitals in the nation,Lauren ended up diagnosing her own POTS by going to the internet, and then getting it confirmed by her doctors.
The POTS diagnosis, while a relief, was just the beginning of an ongoing battle with the medical profession to dig deeper.
Small Fiber Neuropathy
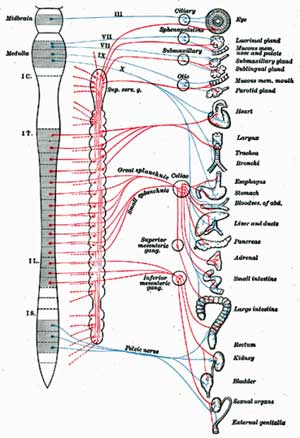
Damaged autonomic nerves across Lauren’s body were causing her POT, digestive issues, fatigue, pain, etc.
Lauren’s nerve damage was discovered by accident. While looking for an immune system disorder called mastocytosis, the doctors found that 80% of her sudomotor nerves, the small fiber nerves that controlled blood flow to the skin were damaged or missing. She had, her pathologist said, a “profound autonomic neuropathy.”
These nerves should have been telling her blood vessels to’ tighten up’ when she stood, which helps return blood flow to the heart against the force of gravity. Instead they were letting blood pool into her legs. The subsequent lack of proper blood flow to her brain was causing her heart to race in an attempt to restore normal blood flow to her brain.
Medical Roadblocks
Nerves don’t just spontaneously combust. -POTSgrrl
Finding her small fiber neuropathy (SFN) was a big step forward, but getting her doctors to act on that finding was something else indeed.
It’s not possible to determine the cause of POTS or SFN in many cases, but that didn’t mean, she felt, that doctors shouldn’t at least try. After all the pain and misery she’d been put through, she felt they should at least do that… but most of them were reluctant to do so.
“I saw numerous so-called “POTS experts” who told me there was no way to identify the cause of my POTS and that I shouldn’t bother looking because it was just “idiopathic.” They also said it would “probably just go away on its own in 5-10 years.” POTSgrrl
In fact, many things can cause SFN and it’s not always possible to find a cause, that doesn’t mean you shouldn’t try.
“It’s just a matter of your doctors and you working really hard to figure it out. Modern medicine does have its limits, so not everyone will figure out what is causing their POTS, but it is sure worth a 110% try if you are as sick as most POTS patients.” POTSgrrl
She refused to rule anything out until tests actually ruled it out.

The missing piece for Lauren was a lip biopsy. Despite testing negative on numerous autoimmune tests, her lip biopsy revealed she had Sjogren’s Syndrome.
It was not easy. When she didn’t test positive for the antibodies associated with Sjögren’s Syndrome (SS-A, SS-B and ANA), she was told that wasn’t it. One year and many neurologists later, Dr. Kamal Chémali, a neurologist at the Cleveland Clinic (who’d recently opened up a new autonomic lab in Norfolk, Virginia), finally gave her the full workup she needed. When Lauren questioned the need for a minor salivary gland lip biopsy, because her prior neurologist had “ruled out” Sjogren’s due her negative antibody tests, Dr. Chémali, told her that approximately 40-70% of people with Sjögren’s do not test positive for the typical Sjögren’s antibodies, and that a minor salivary gland lip biopsy was the gold standard test.
Although all of the other Sjögren’s related antibody tests had been negative, her lip biopsy revealed she had Sjögren’s Syndrome. Despite having the term “syndrome” in it’s name, enough detail has been discovered about Sjögren’s that it is now considered a specific disease.
The POTS Puzzle
POTSgrrl (Sjögren’sgrrl?) eventually discovered that an autoimmune disorder, Sjögren’s Syndrome, was the cause of her POTS. Sjögren’s Syndrome isn’t the only autoimmune disorder that can cause POTS or other forms of autonomic dysfunction. Lupus, Anti-Phospholipd Syndrome, Guillain Barré Syndrome, Chronic Inflammatory Demyelinating Polyneuropathy, Multiple Sclerosis, Crohn’s, Addison’s and Graves’ Diseases and, Hashimoto’s Thyroiditis, can cause or be associated with autonomic neuropathy, which can sometime present just like POTS.
In addition to autoimmune disorders, Diabetes, endocrine abnormalities, severe deconditioning, infections, genetic disorders, inflammatory disorders, Ehlers-Danlos Syndrome, connective tissue diseases, head, neck and spinal cord injuries, and pregnancy can trigger POTS or POTS like symptoms as well.
Sjögren’s Syndrome
Lauren’s POTS was caused by SFN impacting her autonomic nerves.Sjögren’s Her SFN was caused by Sjögren’s Syndrome. Instead of an ‘idiopathic’ (no known cause) syndrome, she had specific autoimmune disease that was attacking her autonomic nervous system as well as some of her major organs.
Lauren actually got diagnosed fairly quickly. It takes the average Sjogren’s patient six years to get diagnosed. Sjogren’s is the second most common autoimmune disease in the US, behind rheumatoid arthritis, with an estimated 4 million suffers, but only 1 in 4 is diagnosed.
Lauren was persistent–and fortunate–to finally find a neurologist, Dr. Chémali, willing to do a full workup. One wonders how many POTS or ME/CFS patients are willing and able to so consistently buck their doctors opinions.
POTS can be caused by many different things, but Lauren believes a significant number people diagnosed with POTS may have undiagnosed Sjögren’s.. Like POTS, Sjögren’s predominantly impacts women. Studies suggest that small fiber neuropathy is often the first problem to show up in Sjögren’s, while the antibodies doctors typically associate with Sjögren’s often show up later or not at all. Few doctors, however, test for small fiber neuropathy. If you don’t have dry eyes and dry mouth. you’re probably not going to get tested for antibodies to Sjögren’s, and you’re certainly not going to get a lip biopsy. That suggests that a subset of younger women with autonomic nervous system problems who have early or atypical Sjögren’s probably aren’t getting properly diagnosed.(—–incorporate Dr. Birnbaum info this paragraph—(
Sjögren’s Syndrome typically attacks exocrine glands that produce moisture in the mouth, eyes, sinuses, gastrointestinal tract, and lungs, but the centeral and peripheral nervous system can be impacted as well. Sjögren’s Syndrome whacked the salivary glands in my mother so hard that they looked like bananas, but the real damage came when it attacked her kidneys.
Often considered the hallmark symptoms of Sjögren’s , dry mouth and eyes are not always seen. Despite her horrifically disturbed autonomic nervous system, Lauren had only mildly dry eyes and no dry mouth at all.
This is a very variable disorder. Let’s take a look at how Sjögren’s can present.
Symptoms
There is no organ, system or tissue in the body that Sjögren’s cannot impact, although no patient has every possible symptom. The most
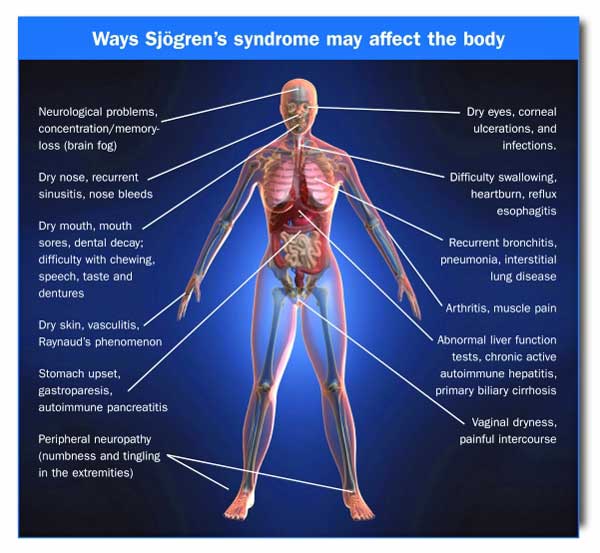
The second most common autoimmune disorder in the US, Sjogren’s Syndrome is often misdiagnosed as ME/CFS or fibromyalgia. This image is from the Sjogren’s Syndrome Foundation’s website.
common symptoms of Sjögren’s are dry eyes, dry mouth, fatigue, joint pain, muscle pain, small fiber neuropathy pain or numbness in the feet and brain fog. Sjögren’s can produce many other signs and symptoms including shortness of breath, frequent dry coughing, dry stuffy sinuses, sinusitis, canker sores, nosebleeds, oral infections, cavities, receding gums, difficulty speaking or swallowing, salivary gland swelling, acid reflux, heartburn/GERD, cramps, reduced gut motility, nausea, vein swelling, dry skin, itchy eyes, stinging pain in the eyes, eye infections, blurred vision, painful intercourse, vaginal dryness, yeast infections, swollen liver, primary biliary cirrhosis, reduced liver functioning, central nervous system impairments, lesions on the brain, … a large collection of signs and symptoms that reminds one of how difficult a diagnosis can be.
The fatigue experience in Sjögren’s is apparently similar to that found in ME/CFS. Lauren described her fatigue in a quite ME/CFS-like manner.
I gave this (fatigue) a category unto itself because it doesn’t fit neatly into any other category. It is a fatigue that is not relieved by rest and sleeping. You can sleep well for 10 hours, and wake up feeling like you just got run over by a truck.
The best description I have heard is someone who said it feels like you have the flu every day, or it feels like you have been beaten up by a thug. When the fatigue hits me bad, I feel like I have cement shoes on and bowling balls tied to my arms and head. It takes great effort just to get out of bed or stand up from a chair. – POTSgrrl
The Diagnostic Dilemma
A couple of things get in the way of diagnosing these conditions correctly. Since ME/CFS doesn’t fit into a recognized medical specialty like rheumatology, most people with ME/CFS probably get diagnosed by general practitioners who don’t have the background to understand or treat the disorder. People with fibromyalgia with POTS see rheumatologists who don’t have a clue about the autonomic nervous system. After they get past the psychologists for anxiety disorder, most POTS patients probably next see cardiologists, most of whom know little about POTS.. As Lauren learned more about POTS and her nerve damage, she realized she needed a neurologist specializing in autonomic neurology.
They’re rare–she thought maybe 50-100 were present in the entire country–but their level of expertise is variable; before she found good nuerologist at the Cleveland Clinic, Lauren went through several neurologists who seemed to know less about POTS than she did. One absurdly recommended that she get used to being sick because “there is nothing we can do for you people.”
Her communications with other patients led Lauren to realize that many people with POTS who have autoimmune issues are not getting the help the need, and many people with Sjögren’s Syndrome who have autonomic nervous system (ANS) issues are not getting the help they need either. (Since other autoimmune disorders can affect the ANS as well, you can throw in Lupus, MS, etc., patients in there). Lauren found that women on Sjögren’s forums frequently reported dizziness, fainting, and rapid heartbeat when they stood up–all potential signs of undiagnosed POTS or another form of autonomic dysfunction
If that’s so, you can bet your bottom dollar that many more people diagnosed with the biggest ‘wastebasket disorder’ of them all–chronic fatigue syndrome—or fibromyalgia with autoimmune or autonomic nervous system problems are not getting diagnosed.
Just last year two studies, both authored by Dr. Julia Newton, strongly associated Sjogren’s Syndrome with autonomic nervous system problems, and helped clarify the ANS connection in that disorder. Dr. Newton has been uncovering autonomic nervous system issues in ME/CFS, Sjogren’s Syndrome, and liver disease.
Next up
Lauren’s POTSgrrl blog is a gold mine of good information on POTS, Sjögren’s Syndrome, and autonomic nervous system dysfunction, and we’re going to continue mining it. Lauren highlighted how important patient education is in these disorders, and with that in mind we’re going to ask: “Could I have autonomic nervous system dysfunction, POTS, or Sjögren’s Syndrome?”, If the answer to that is yes, we’ll see what one very informed patient, Lauren, suggests you might do next.
We’ll also be looking closer at Lauren’s unusual treatment approach which paid off – not with complete health –but with very substantial gains.
In 2012 Lauren created a non-profit; Dysautonomia International to support research and foster a better understanding of the often hidden autonomic nervous system disorders among us. The Dysautonomia International website offers information on POTS, doctors that specialize in diagnosing and treating autonomic disorders, and ways to get involved with research.










Great article! I always wonder how many “subcategories” of ME/CFS are due to lazy doctors and poor diagnosis!
I’ve never been able to get a 2nd opinion, UCSF, Stanford, anywhere!
Glad we got one out you liked Gregory (:))…
Lauren’s story is a big eye-opener for me and I’m going to pursue the dysautonomic/autoimmune connections further in future blogs. It’s going to be interesting…
I have been down a long battle of struggling for many years now. I’m 29, with interstitial cystitis, eosinophilic esophagitis, endometriosis that resulted in a full hysterectomy at the age of 24, bilateral hip surgery, fibromyalgia, POTS and neurocardiogenic syncope. I have 12 specialists and have been to Cleveland clinic. I get chronic hives, severe fatigue, pain everywhere, GI issues, painful urination, prone to pyelonephritis, brain fog, memory loss, rashes, sensitivity to cold, swelling in feet/ankles, insomnia.. and the list goes on. I’ve had positive and negative ANAs so my rheumatologist said there’s no way I have an autoimmune disorder (hence the garbage diagnosis of fibromyalgia) my dad had all of the same symptoms and passed away last year at 53yrs young. I keep telling the doctors, they have to all be connected to one thing… all inflammatory responses! No one will look into this! Not even Cleveland clinic. I’m exhausted seeing so many doctors and finances are terrible… they just keep piling more meds I cannot afford. I just want to be a good mom to my 8yr old and most of the time I cannot even keep my eyes open or roll out of bed.
Can you give me guidance? How did you have the will to continue to figure things out? How do you find the right doctors to take you seriously? Cleveland clinic in Ohio treated me like a hypochondriac. My electro physicist is the only one who seems to care, but he can only do so much. Any advice would be appreciated. Thank you
I’ve been dealing with “DFS” (Doctor Fatigue Syndrome), but now wondering if this is something I should pursue. Yeah, exactly, at some point you’re tired of waiting for the next float on the endless doctor parade and just decide this is CFS/ME-related — nothing else can be done. Very interesting and great to know. You’re the best, Cort — thank you!
A couple of things I got from Lauren’s story
(a) she was a great researcher; despite her physical problems she was still doing OK cognitively and she researched the heck out of POTS
(b) she was lucky to accidentally get that diagnosis of nerve damage
(c) that diagnosis is actually quite daunting since so many things can cause it but once she got it she wouldn’t rest until she clicked all of them off her list
(4) she kept going until she found a doctor (Chemali) who was willing to do the tests needed; she didn’t give up. One of the things we’re going to do in the next blogs is figure out how to find good doctors. This is, after all, a fairly new field and even some of the putative experts are suspect.
(5) she was one of the people with small fiber neuropathy who was unable to find a cause and get significant help….she was very persistent!
This is fascinating. I am writing an ME book at the moment, part lyrical essay, part memoir, and this kind of story just keeps me going because I realise I am not the only one who appears to be in some Kafka-esque nightmare, with doctors not having a clue. Would it be possible to use your story (summarised from here) as an example of that?
Kafka-esque is a good way to put it. I put the blog together largely from things wrote on her blog. You can find Lauren at Dysautonomia International is you want to get in touch with her. Good luck with your book! and your journey :).
Hi Tanya,
I am writing as well about ME right now. Would you like to connect about our projects? I would like to know more about your approach. It looks similar to mine. If you like, Cort can connect us. Thanks, Cort.
This was a very interesting article and shows we should keep looking for answers, and maybe we will learn something from connecting to people with other disorders that will bring us that breakthrough we need.
Very interesting. Many thanks. How is SFN tested for please?
There’s some information on this blog – http://www.cortjohnson.org/blog/2013/08/06/small-fibe-nerve-study-suggests-new-era-in-fibromyalgia-and-perhaps-chronic-fatigue-syndrome-may-be-at-hand/ – but it’s not complete. I’ll get into more on the testing front in the next set of blogs.
We all know that good physical health is no bulwark against ME/CFS/FM/POTS/Sjogren’s but this was ridiculous. This was a woman who could beat the boys at their game; she was a snowboarder, skier, trekker, hiker, etc…..she was out there tearing up the muck….and she was laid as flat as a pancake in just 4 days – amazing!
We all look at infection in ME/CFS but Lauren’s case shows a strong autoimmune response can do the same thing just as fast….and…you can have a horrific autoimmune response and still not test positive to ANY ANTIBODY TESTS…
That’s both scary and exciting to me. …It kind of opens things up 🙂
Thank you for this article. I follow your blog but was unfamiliar with your in-depth history. My daughter, age 14, has POTS and is under the care of a physician at Duke University Hospital. We have had some success recently. She has Ehlers-Danlos, having just been diagnosed at Duke in January, 2013. She became ill in January, 2011, ironically enough, upon return from a ski trip. She has been out of school most of the time since she became sick. She starts high school tomorrow – at a new, private school that has promised to accommodate her ever-changing needs; we are hopeful.
I look forward to learning even more to help her in the future. Perhaps testing for Sjogren’s is part of that as her paternal grandmother does have Sjogren’s. Does the clinic in Cleveland see teens or just the over 18 crowd?
Thank you for sharing your journey and for your advocacy for those on the same road!
I imagine the Cleveland Clinic sees teens but I don’t know. Lauren – who’s history I wrote about in the blog would know – I would encourage, you, though to talk to her doctor and find about a lip biopsy. I’m a male, I don’t have dry mouth or dry eyes but my mother had Sjogren’s Syndrome and I’m considering a lip biopsy.
We’re going to have a blog coming up shortly that will look at EDS a bit……
Good luck with your daughter!
Cort, I have a friend that is male and has POTS and he was just DX’d with sjogren’s with a lip biopsy. It was not picked up any other way. Also, another guy with POTS also found that he has SFN and he also has AS (ankylosing spondylitis). Even though POTS is mainly female – there are males with this too.
So, just because you don’t seem to fit the mold or picture – don’t rule it out until it’s ruled out.
Issie
OMG….That would really be something….
I should get this checked out….
Thanks
Yeah, you should! Let us know. We are all looking for that one piece that might make things make sense. I’ve had a couple of “light bulb moments” of discovery and it’s exciting when it happens.
Issie
I have to warn you that the Cleveland Clinic is not the end all- be all of diagnostic perfection. From my experience, I would tell you to insist, emphatically, not to be pawned off on a student doctor. My visit did include a brief visit from the attending but the rest of my case was handled by a child (relatively speaking) and ultimately dismissed. I could easily poke massive holes in her logic regarding my case but it wasn’t worth the effort. Good luck arguing with a “doctor” :). I wish you luck though.
Here is a more recent paper on autoimmune issues and neuropathy. It’s a little unsettling – but, not a surprise to me.
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3703364/
Many of us with POTS are connecting autoimmune issues. Many of us, especially with EDS (Ehlers Danlos) also have MCAS (Mast Cell Activation Syndrome) and GastroCrom works by not only stabilizing mast cells but working on the immune system at the intestinal level. (This was probably Lauren’s findings when she was being tested for mastocytosis. As this has been what the majority of us find when we go through this testing.)
I feel there is a genetic component to this – mostly because of my family history. My sister has OI and CFS and all three of her children have some form of dysautonomia. I have HyperPOTS, MCAS and EDS and also vitiligo, alopecia and hypogammaglobulinemia. With my mom having sjogrens and probable MCAS and Dad having Guillian Barre and neuropathy on both sides of my family and my grandparents having shown signs of some of these things -yet never DX’d –it just seems there is a genetic connection. My POTS doctor at Mayo feels that many of us have autoimmune problems that science can not yet pick up.
On the blog that Cort referenced, there are things listed that can be done for autoimmune problems. Despite being offered IVIG – I’m trying to do it with more natural type things – listed on that blog. (Diet, low-dose antibiotics, antimalarial herbs, colostrum, turmeric, astaxanthin and more).
I’m so happy that some of us have been able to keep our “brain function” (at least some of the time 🙂 ) in order to research and try to put things together. There are some wonderful people who have been a good support and we are trying to keep each other motivated to continue researching and supporting one another. Thankfully, we also have some good doctors who are trying to sort this out for us. Just in the 3 years that I’ve been researching, so much has been discovered and we are coming up with ideas that seem to fit and we are getting doctors on board with testing us for these things. If it weren’t for the POTS communities that we form and the internet there would be a lot of people lost in the sea of unknowns, with a lot of wrong diagnosis and those not getting any relief or HOPE. Some of the sites are a place where people can go and just not feel alone. It turns into a place to share things that others can’t possibly understand unless they have it themselves. But, in addition to the support —there is lots of research.
Thanks for helping us spread the word about this Cort. I feel that there are many CFS people that may have this as one piece of their puzzle and that was my goal for coming to your site (in addition to continue learning) —to hopefully – help others find more pieces of their puzzle. I know how miserable it can be and we all need answers. The more people that are aware of what we have and what we are going through – the more chance we have of getting research behind this and finding those answers that we so desperately are searching for. THANK YOU!
Issie
Thanks Issie. I knew about POTS but had no idea about the nerve fiber neuropathy and the autoimmune connections…Rituxian (Rituximab) is now being used with some success in Sjogren’s and ME/CFS…..It seems all interconnected…It’s going to be interesting 🙂
Thanks for the tip for the Forums. With your family history I think you were fated to come down with these disorders – your family is packed with autonomic problems…
Yes, my doc says that if they can get some research money and can do some testing with a family connection – we will for sure be contacted. For years, people have suffered with this thing or that thing – but, never putting it all together or getting down to the “core” issue. Now as science and medicine is advancing – I’m very hopeful that the “core” issue will be discovered and something can be done about it. At least maybe we can have a little more quality of life. With epigenetic advancement and all the new research in genetics, and the continuing discoveries with autoimmune issues – maybe there will be some answers. Hopefully, in my lifetime.
Issie
Hey Cort, great report! I just sent blood work to Miami and Sjogren’s is being tested for the first time. My eyes are itchy and dry and mouth dry. Interestingly, I woke up one morning in the 80’s with a burning tongue and no one could tell me why .I was not sick the first time until 93 after the flu shot.
I have seen the burning tongue on lists of symptoms of EVB.
There are two doctors here Pridgen and Duffy that have the theory that small nerve neuropathy is EVB hiding there. They are conducting a study now their story is on Google.
I am anxious to read Lauren’s blog, thanks Lauren for sharing.
I will be calling tomorrow about a phone consult about my blood work and I will be very surprised if I do not have Sjogren’s. I would prefer allergies which is usually diagnosis.
I will post the results.
Thanks Marg,
Good luck with the test – however it turns out…its kind of two-edged sword isn’t it. Who wants an autoimmune disorder? On the other it may open up some options. If the test comes back negative remember that you can SS and have a negative test; the lip biopsy is the only definitive test.
I’ll look up Duffy and Pridgen – thanks 🙂
Hi Cort.
Thank you for an interesting post. This is my notes on the subject:
Assessment of prevalence and pathological response to orthostatic provocation in patients with multiple sclerosis
http://www.ncbi.nlm.nih.gov/pubmed/23127354
Autonomic dysfunction in multiple sclerosis presenting with postural orthostatic tachycardia
http://www.ncbi.nlm.nih.gov/pubmed/23160808
Postural orthostatic tachycardia syndrome associated with multiple sclerosis
http://www.ncbi.nlm.nih.gov/pubmed/23246200
Autonomic dysfunction presenting as postural orthostatic tachycardia syndrome in patients with multiple sclerosis
http://www.ncbi.nlm.nih.gov/pubmed/20309394
Postural orthostatic tachycardia syndrome in a patient with relapsing-remitting optic-spinal multiple sclerosis: A case report and discussion of possible mechanism
http://www.neurology-asia.org/articles/neuroasia-2012-17(2)-155.pdf
The prevalence of Neural Mediated Hypotension (NMH), first stage, in SLE patients was 47.9%. Seven patients had both NMH and postural orthostatic tachycardia syndrome.
Ref: Neurally mediated hypotension in systemic lupus erythematosus patients with fibromyalgia
http://www.ncbi.nlm.nih.gov/pubmed/14983104
Autonomic dysfunction in fibromyalgia syndrome: postural orthostatic tachycardia
http://www.ncbi.nlm.nih.gov/pubmed/19007537
Autonomic nervous symptoms in primary Sjogren’s syndrome
http://www.ncbi.nlm.nih.gov/pubmed/18411214
A sicca syndrome clinically indistinguishable from Sjögren’s syndrome also develops in a considerable proportion of patients with organ-specific autoimmune diseases, such as primary biliary cirrhosis, multiple sclerosis or gluten-sensitive enteropathy , and in other chronic non-immune-mediated illnesses, such as fibromyalgia or chronic fatigue syndrome.
Ref: Dry eyes and mouth syndrome–a subgroup of patients presenting with sicca symptoms
http://www.ncbi.nlm.nih.gov/pubmed/11961172
Halle Nielsen, this is great! Can I recruit you to be a volunteer for the Dysautonomia International research team? We have a group of volunteers who compile the most relevant journal publications for us on various topics, and then we post those articles or at least the abstracts on our website on a regular basis. If you are interested, you can reach our Research Coordinator, Carrie, at info@dysautonomiainternational.org.
Sincerely,
Lauren Stiles
a/k/a POTSgrrl
This makes a lot of sense. It seems that this is basically what the Gulf War Illness docs are saying. When there is persistent, unexplainable issues with HR/BP/Breathing, etc, ANS should be investigated and thought to be the cause. “Stress” and “anxiety” and other non-descriptive nonsense need to be relegated to the bin of quackery and incompetence/laziness.
Hi Cort,
I am so honored that you decided to write about my story. I have been a fan of this website for some time, and I was thrilled when I saw your message in my inbox a few days ago.
Many of the details of my symptoms were facts that you gathered from my POTSgrrl blog, which I wrote during the two years that I was mostly bedridden. I would discuss different symptoms on different blog posts. I never compiled all of my symptoms into one giant list. Your article put almost all of them together in one place. Reading someone else’s description of my mile long list of symptoms was emotional for me. It reminded me of how sick I really was, and how thankful I am to be feeling so much better (not 100%, but definitely better than I was).
I am fascinated by the comments posted below your article, and I will try to respond to comments directed at me when I have some time to think of witty and inspired answers.
Since this article was published two days ago, Dysautonomia International has been contacted by dozens of people who also have POTS and Sjogren’s, or POTS and Lupus (which I lovingly refer to as the evil cousin of Sjogren’s). Most of them have never had a doctor explain that their autonomic neuropathy/POTS/dysautonomia symptoms were likely caused by their autoimmune disease. This is something that needs to change.
There are so many people out there who have autonomic neuropathy as a result of autoimmune diseases. We all know how hard it is to get diagnosed when you have an autoimmune disease. Then add to that how much harder it is to find a doctor with enough expertise to diagnose and properly characterize autonomic dysfunction, and what to do about it. I am hoping that we can improve that situation in the near future, by educating medical professionals about autonomic disorders, training up and coming medical professionals to become experts in this field, and increasing awareness amongst the general public. These are three things we are working on at Dysautonomia International.
Thanks so much for highlighting a broader issue facing the chronic illness community – the difficulties we face in trying to obtain a proper diagnosis. My “misdiagnosis misadventure” may sound shocking to people who have been blessed with good health or who have an easy to diagnose disease, but I know that many other patients with complex or chronic illnesses have been through the same thing I have, and sometimes much worse.
I look forward to reading you future articles about the autonomic nervous system, and everything else you write about. Keep up the good work!
Sincerely,
Lauren
Lauren,
How are you doing since you’ve been addressing your autoimmune issues?
Is there a way to connect to the group if one doesn’t want to do Facebook or Twitter? I’ve had several people tell me about the group and they all seem to really be enjoying it. Would you provide a link?
Issie
I dont actually have a clue what pots is but im going to research it tonight. I have been dx with fibromyalgia, cfs. ive been thinking I have sjogrins for a long time but I havnt ever been checked for it nor has my doc offered to check. I have lots of joint pain was the reason and dry eyes. I have many more symptoms since ive read this blog that I didnt know were the symptoms. thanks so much for all of this. looks like I have lots more research to do.
Good luck on your search, Becky!
I just have to tell my news. Since I’ve been working on my immune system for about 7 months now and we know there are autoimmune connections with my POTS and other things – I’ve reversed chronic kidney disease from stage 3 to nearly stage 1. At stage 4 they start to talk to you about dialysis. It’s pretty much unheard of to reverse kidney disease.
And today, I got my eyes checked and my vision has improved. So much so that my glasses and contacts need to be decreased in correction. I asked if they have ever seen that happen and they said not with a person who is nearsighted. The doctor wanted to know what I was doing and said to stick with it. She was thrilled that I’m having these improvements.
Also, I saw some family that I’d not seen in about 5 months and they couldn’t believe how well I’m doing. They said I look like a different person, both in my appearance and how well I’m functioning. My sister-in-law said that I look the best that she has ever seen me, and that’s in 20 years.
I think that my low-fat vegan diet has played a big part in my improvements. And also the things I’ve been doing to address my autoimmune system. Just thought it may give others hope. I’m going in the right direction. Yayyyyy!!!
Issie
Lauren and I are incredibly similar. In addition to being distant cousins (we share a maternal ancestor many generations back), we share a remarkably similar genome, particularly the immune system portion (83.25% in common). We share an astounding number of diagnoses. Clinically, I have Sjögren’s…I am slated to see Dr. Chemali (Lauren talked me into it, and I am grateful) in January for the lip biopsy as final confirmation. I have a personal theory that something about this storm of conditions (I call it Zebra Soup) seems to mess with the typical bloodwork for autoimmune conditions (ANA, RH, etc)….something masks the typical elevated counts doctors look for. I also clinically have RA, but test fine on the bloodwork. It runs in both sides of my family and my genome is riddled with risk alleles for both RA and Sjögren’s. I also have Vitiligo, an autoimmune condition causing depigmentation of the skin. These three conditions very often cluster, I ought to mention.
I also have SFN and Erythromelalgia (both found on the same gene) as well as RLS, Reymaud’s, two forms of Dysautonomia (POTS and NCS/NMH), and several debilitating degenerative spine conditions. Where we differ is that, to her knowledge, Lauren doesn’t share my Ehler’s Danlos.
Because of our similarities, I am hoping that I might find some improvement with similar treatment. Lauren has been a great help to me 🙂
Shae
http://www.ZebraSoup.com
Shae,
Okay, so you and I have similar things. I have vitiligo and alopecia and low IGG levels (hypogammaglobulinemia) and tested positive for dsDNA (Lupus markers – but last test was negative). I have EDS and AS (ankylosing spondylitis). And HyperPOTS and MCAS. I have osteoarthritis and FMS. So far, not testing positive for RA. Hopefully, will not. My mom has Sojourns and my dad Guillain Barre and neuropathies are on both sides of my family. I’m sure there is a genetic component with all these things. I know there is with some of it. It would be interesting to compare notes with you and Laureen since we all have POTS and similar issues. Are you on 23&me?
I haven’t been tested for sojourns myself – but, do occasionally have dry eyes. I have problems with neuropathy (but since I’ve been working on my autoimmune system that is getting better.)
I wish we could figure out the link —other than bad genetics. I am however, getting a whole lot better with what I’m doing.
Issie
Hi Isse,
To answer your question from above, the best ways to get in touch with Dysautonomia International are by checking out our website (www.dysautonomiainternational.org), “Liking” our Facebook page (www.facebook.com/dysautonomiainternational), following us on Twitter (@Dysautonomia) or e-mailing us at info@dysautonomiainternational.org. We don’t run a forum or chat group, but many of our volunteers are active on the largest POTS Facebook group, which can be found at:
https://www.facebook.com/groups/75183049224/.
I also wanted to gently encourage you to get tested for Sjogren’s. A few of your comments about your symptoms/signs on here raised my eyebrows. Hypogammaglobulinemia can be seen in Sjogren’s. Sjogren’s runs in families, like most other autoimmune diseases. Some genetic markers have already been identified that increase your risk of developing Sjogren’s. Dry eyes, even mild, can occur in Sjogren’s. Your sporadic Lupus markers and ank spond diagnosis also raised an eyebrow, as about 50% of Sjogren’s patients have a second or third autoimmune disease, with RA and Lupus being the most common ones, along with Hashimotos. I’m not an expert on kidney matters in Sjogren’s, but I know it can cause significant kidney problems in some patients.
Even though you already have more than your fair share of health conditions, it’s still helpful to have Sjogren’s confirmed or ruled out. If you have it, there are specific treatments that can really help, and it’s important to prevent damage in the future, because Sjogren’s is slowly progressive. As I’m sure you know, it’s much better to prevent or slow down joint or nerve or eye damage now, than to have it slowly get worse over time until you end up really debilitated from it and it can’t be reversed.
Healthy eating and lifestyle habits are really important for any chronic health condition, but if you have Sjogren’s, there are other things that you can add to your regimen to help prevent the damage from getting worse. I don’t want to sound down on dietary/lifestyle changes, because I think they are essential and I do them myself, but even a perfect diet/supplements/healthy lifestyle is unlikely to stop the progression of Sjogren’s, so it’s really important to get diagnosed early and get on the ideal medications, while continuing all of the other healthy things you are doing. We need every weapon we can find to fight this beast.
Best,
Lauren
Thanks for the suggestion Lauren. If what I’m doing with my immune system stops going in the right direction, I will consider more testing. I’m working on it pretty aggressively right now and I’m seeing good improvements.
My mom has sojourns and it very well could run in the family. I have genetic markers for it already.
Thanks for the links.
Issie
Did all of your symptoms, by chance, begin after taking a fluoroquinolone antibiotic – Cipro, Levaquin, Avelox, Floxin, etc.? Adverse reactions to these drugs are often delayed, with initial symptoms starting weeks or months after administration of the drug and often getting progressively worse over the years, so it’s difficult to connect the cause, the drug, to the effect, body-wide breakdown. Fluoroquinolone antibiotics, Cipro, Levaquin, Avelox, etc. are DANGEROUS drugs. These popular antibiotics, 26.9 million prescriptions for fluoroquinolones were written in 2011 (per the FDA), can cause damage to connective tissue (tendons, ligaments, cartilage, fascia, etc.) throughout the body, damage to the nervous systems (central, peripheral and autonomic), and more. They disrupt and damage DNA, cause mitochondrial malfunction and increase oxidative stress throughout the body. They cause a massive decrease in important antioxidants like glutatione and superoxide dismutase (SOD) and increase production of lipid peroxide and reactive oxygen species (ROS) that result in cell death. CELL DEATH. There is no known cure or treatment for those who are suffering from the adverse effects of these drugs.
Please note that adverse reactions to these drugs often look a lot like an autoimmune disease. When my adverse reaction began, I thought that I had Lupus, RA, MS, Sjogrens, etc. These drugs also cause crippling exhaustion and damage the autonomic nervous system.
Please, please, please look into it. Thank you.
Lisa, so how did you figure out the antibiotic contributed to your illness? What are you doing for it?
Issie
Hi Lisa, are you still following this link as I have a similar story?
Please LMK…thanks Colleen
This story has brought me to tears as all so familiar my partner said sounds like I wrote it and there isn’t enough pages let alone my hands handle before crampingto tell my story that is basically identical although being diagnosed also through Drs specialists rheumatologist cardiologist lung specialists you name it so many issues steamrolled that I just told to manage it when I can feel my body being eaten away and mentally I am flowing due to twelve years of this vicious cycle from fibromialgia to disc degeneration to pots to lung issues to spine feeling like no matter hoe much I fight an strengthen it I wake weaker by the day.. losing career after career after working so had through this he’ll to make it where I would be to then have to walk away.. .havingto have abortion this month has tipped me mentally over edge as after everything can’t even enjoy that feeling of motherhood which would give me reason to keep fighting.. I Have wasted thousands and thousands on treatmentfor symptoms to go in circles and be dumped in the too hard basket.. after heart failure two YeaRS ago in Thailand on my first holiday at 30 yrs of age and have my partner and I say our goodbyes never thinking I would make it back only to fall apart more.. I feel if I gave up I already dead and therefore cannot.. it is impossible to find an educated specialists who won’tlook for quick way out to get you out those doors quicker.. it’s an awful feeling and you loose yourself in he’ll.. I cry knowing so many people in this position crying right now feeling alone when there is help out there even a healthy person would find this exhausting battle hard.. anyone Have any specialists contacts in Melbourne Victoria please help. Thank u Kristen
My heart is going out to you. Im in Australia too, SA for me and very bad as well and in fear that this illness will kill me.
Ive had to be ambulanced to hospital this year again due to my POTS.. heat knocked me around and I just couldnt recover with the warm weather, I was on the floor and couldnt even crawl. Passing out isnt abnormal for me with my POTS but usually I recover after being on floor or ground for up to 45 mins.. but on this day being warm, it wasnt going to happen, I would of been on the floor all night and the next day too. I believe I’d be dead right now if one of my support workers (I have them come in twice per week) hadnt been there to ring ambulance.
At the hospital, my blood tests showed I was very dehydrated to the point that my kidneys had stopped functioning properly (thou I’d drank 5 L that day!).. impossible in warm weather for me to keep my hydration (if I drink 6-7L in one day I start vomiting). With the POTS my body doesnt hold its fluids well and I feel like I just pee out what I drink thou my florinef does help some but no where near enough (I cant go out alone ever due to Im too at high risk of collapse).
The hospital gave me 2 bags of saline by IV. (at the hospital my resting heart rate had gone up to 140/150 and my BP was up to 180 due to the bad POTS attack.. the saline IV brought them down. Thank God I struck an emergency doctor who believed me when I told him I had the hyper noradrenalic kind of POTS and then went and looked up what to do online and decided to give me IV even thou my BP was high!
Crazyily when I saw a specialist in autonomic disorders.. a professor, at the main states hospital and supposely specialising in POTS.. she dismissed that I could have POTS due to the fact I get orthostatic hypertension as I have the hyperadrenalic kind of POTS which she knew not a thing about!!! She she dimissed me just telling me to drink more if I believe I have POTS (when I already have to over drink to the point my electrolites have become very screwed up at times).
The hospital emergency dr due to fearing for my kidneys due to the results of my blood test and my dehydration.. told me to increase my Florinef up to 4 times higher then my current CFS specialist allows me to do. So now Im having to do that and arent even being monitored for my potassium levels with this which are supposed to be monitored if one is on Florinef.
My CFS doctor who does know a little bit about POTS got to the point with my POTS in which he didnt know what else to do with me and didnt feel comfortable doing anything a more aggressive with it. I only get about 10% improvement with my medical compression stockings to the tops of my thighs.. 30% improvement with the Florinef.. but with all this Im still collapsing and can never leave my house alone. So anyway.. its scary knowing my kidneys are suffering each time I get dehydration or are having a big POTS collapse.
Irronically unlike some other states of Australia.. POTS/ME/CFS patients do not quality for the heating and cooling rebate. this state knocked that back thou its available for other heat sensitive illlesses (I have to keep my aircon almost all the time.. I can start getting sicker at only 25 Celicus.. and the hotter it is, the more I struggle with the POTS.
Im currently starting to take legal action for discrimination thou the equal opportunity board of very bad neglect as I cant get home care for these conditions and instead they just give me a wee bit for my mild Aspergers and completely ignore the fact that Im now in a wheelchair quite often and need that every time I go out (and need someone to push me).
.thank you
These stories always start with a biography detailing how active and happy the patient was before getting ill. It seems to add validity to the claim that the illness is purely physiological and not mental and that the patients are not just malingerers.
I’ve been told by 3 MDs that I “have dysautonomia”. I have known for a long time my ANS doesn’t work as it should. I no doubt qualify to be dx with ME/CFS, fibromyalgia, anxiety, and clinical depression. Despite the fact that I have many physical problems not explained by anxiety or depression I believe I still “have” them. I dont believe that I just “appear” to have anxiety and depression because of my nutty ANS but that I do in fact have those illnesses comorbid or secondary to dysautonomia. That is just my experience.
The thing is, I have never been active, vibrant, healthy, and thriving. I’ve always had lower energy, digestive problems, sleep disorders, bladder problems etc. My diagnosis then seemed to be “lazy and whiny kid” with a “nervous stomach.” As I got older more and more symptoms would present themselves such as heart palpitions, chest pain, tinitus, migraines, TMJD, fatigue, exercise intolerance, etc.
These symptoms run in my family as well.
And yet I dont seem to have any of the known dysautonomic disorders. What is one to do if they know they have ANS dysfunciton and yet there doesn’t seem to be an acronym that applies? (other than OI) Is it really worth going through a huge battery of more tests and traveling around the country just to find a better label for what is happening? Especially since whatever is going wrong with me has always been there an runs in my family?
Was this cascade of events triggered by vaccine uptake? Has that been considered, established? http://www.sciencedirect.com/science/article/pii/S156899721300178X
Look up the story of Judy Mikovits, PhD and how she connected Chronic Fatigue to vaccine viral contaminant. They targeted her. The lies continue.
I live in Sydney Australia. does anyone know any doctor in Sydney that I could consult for management/treatment of my condition. most doctors just tell me that there is nothing wrong with me go home and rest. thank you it has been interesting reading the posts here. Norma Jensen
Fibromyalgia pain can be frustrating. I had Fibromyalgia for at least 7 years. In 2015 it really kicked in with widespread pain, soreness, sleeplessness, inflammation and extreme fatigue. I tried so many medications and supplements to get some relief nothing worked, until last year, i learnt about FIBROMYALGIA SUCCESSFUL TREATMENT from Rich Herbs Foundation (RHF). Few weeks into the treatment, I went back to work feeling good and my legs weren’t hurting, i almost forgot how long it has been since I felt this good and normal. The pain was 95 percent gone on my legs and lower back. Visit RHF we b page www. richherbsfoundation. com. Here I am 11 months after the treatment and i still feel good and active.
Thank you for doing what you do. Your blog continues to give me hope
Thanks – I’m glad. It gives me hope as well! 🙂
Has anyone tried vitimmin c iv only thing kills ebv I ahoing to try willlrtu know 33 yr sufferer
Persistent, unexplained dry cough has been added to the list of suspicious symptoms for Sjogre’s.
I received copies of my latest blood work today. Sjogrens Antibody (SS-A) negative at 1.0
Sojgrens Antibody (SS-B) negative at 1.0. My eyes burn and itch and my mouth burns and is dry. So wonder about the lip biopsy and then what is the treatment if that is positive? I do not know anyone here that would do that. Yes, Cort a double edged sword.
Six tests for Coxsackie were negative at 1.8, wonder if I can stop the Equilibrant. I have a phone consult on the 11th. There is moderate bacteria showing. Other than that all the tests were normal and negative. It was a great report. My testing at my visit in May was much better, killer cells up to higher than normal from 5%…thanks Imunivor and LDN. I still have activation of EVB and acute and chronic antibodies. So, don’t know how that is now..I think that virus was my main cause, no one got it and no one would test until I saw Dr. Klimas and the titers were blown off the paper. All that going on and no one would test because everyone has EVB over 30, well not with titers like that. I will have to find out more about Sjogrens though.
I can say I feel quite well, still do not sleep right and still have some pain. I do not feel like I have the flu anymore. What a change!
So people hang on, there are treatments that work very well, have to try a lot of things and find a good doctor. Klimas and Rey, the greatest and my GP here.